In the field of modern medicine, cerebral infarction, as a common cerebrovascular disease, has seen an increasing incidence rate in China year by year, posing a serious threat to people's life and health. Atherosclerotic cerebral infarction (ASCI) is an important type among them, and its pathogenesis is mainly due to insufficient blood supply to local brain tissue caused by atherosclerosis, leading to ischemic and hypoxic necrosis. The clinical manifestations include limb paralysis, hemibody numbness, and loss of language function. If not treated in time, it is highly likely to lead to disability or even death. This article will introduce you in detail to a clinical study on the treatment of ASCI with transcranial ultrasound thrombolysis combined with rosuvastatin, allowing you to gain a deeper understanding of the clinical manifestations of this new treatment regimen.
Research background and purpose
With the continuous changes in people's dietary structure and lifestyle, the incidence rate of cerebral infarction has been on an upward trend year by year. In relevant surveys, cerebral infarction ranks fourth as a single cause of death, making it a key topic in clinical medical research. Currently, transcranial ultrasound thrombolysis and statins are commonly used methods for the modern clinical treatment of cerebral infarction. Transcranial ultrasound thrombolysis can assist in reducing plaques and enhancing the effect of thrombolytic drugs; statins can reduce oxidative stress, regulate blood lipids, and anti-atherosclerosis. This study aims to explore the efficacy of transcranial ultrasound thrombolysis combined with rosuvastatin in the treatment of ASCI, with the hope of providing a more effective treatment plan for clinical practice.
research methodology
(I) General information
The study selected 68 patients with ASCI admitted to a certain affiliated hospital of Zhengzhou University from April 2018 to April 2020. These patients were divided into a control group and an observation group according to the random number table method, with 34 patients in each group. There was no statistically significant difference in general characteristics such as gender, age, and disease duration between the two groups (P>0.05), making them comparable. This study has been reviewed and approved by the Medical Ethics Committee of the Second Affiliated Hospital of Zhengzhou University.
(II) Inclusion criteria
1. Inclusion criteria: meeting ASCI diagnostic criteria; aged <75 years; duration of illness ≤20 days; both the patient and their family members have signed the informed consent form.
2. Exclusion criteria: patients with malignant tumors; patients with other cardiovascular and cerebrovascular diseases; patients allergic to rosuvastatin.
(III) Treatment methods
After admission, both groups of patients were given oxygen inhalation support. For those with high blood pressure, losartan potassium tablets (National Medical Products Administration Approval No. H20133123) were administered at 50mg per dose, once daily; for those with high blood sugar, glimepiride dispersible tablets (National Medical Products Administration Approval No. H20140087) were administered at 1mg per dose, once daily; and aspirin enteric-coated tablets (National Medical Products Administration Approval No. H10960304) were administered for antiplatelet aggregation therapy at 0.1g per dose, once daily.
On this basis, the control group was administered rosuvastatin calcium capsules (National Medical Products Administration Approval Number H20140135) at a dose of 10mg per administration, once daily, for a period of 2 weeks;
The observation group received transcranial ultrasound thrombolysis therapy in addition to the treatment regimen of the control group. Using a transcranial Doppler diagnostic device, the ultrasound probe was fixed at the site of infarction and arterial plaque located through imaging examination. After applying medical disinfectant ultrasound coupling agent between the probe and the skin, the device was activated, with 20 minutes per session and 2 sessions per day, for 7 days.
(IV) Observation indicators
1. Clinical efficacy: After 2 weeks of treatment, the degree of neurological deficit in patients was assessed using the National Institutes of Health Stroke Scale (NIHSS). The total score was 042, with a higher score indicating more severe neurological impairment. The efficacy was determined based on the reduction in NIHSS score: basically recovered with NIHSS score reduction ≥90%; significantly improved with NIHSS score reduction 46% to 89%; improved with NIHSS score reduction 19% to 45%; ineffective with NIHSS score reduction ≤18% or increase. The total effective rate of treatment = (number of basically recovered cases + number of significantly improved cases + number of improved cases) / total number of cases ×100%.
2. Blood lipid levels: Before treatment and after 2 weeks of treatment, 5ml of venous blood was collected from the patient in a fasting state. The blood was centrifuged at 3000r/min for 10 minutes to separate the serum. The levels of triglycerides (TG), total cholesterol (TC), low-density lipoprotein cholesterol (LDL-C), and high-density lipoprotein cholesterol (HDL-C) were measured using an automatic biochemical analyzer.
(V) Statistical methods
Data were analyzed and processed using SPSS 20.0 statistical software. Measurement data were expressed as (x ± s) and t-test was applied. Enumeration data were expressed as rate and χ² test was applied. The significance level was α=0.05, and P<0.05 was considered statistically significant.
Research findings
(I) Comparison of clinical efficacy between the two groups
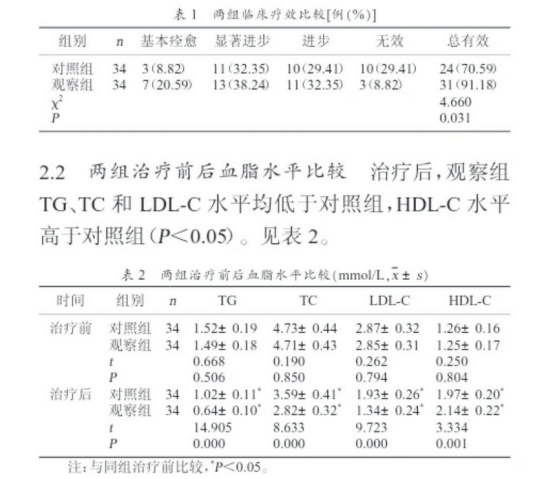
The results showed that the total effective rate of treatment in the observation group was 91.18% (31/34), which was significantly higher than that in the control group (70.59% (24/34), with a statistically significant difference (P<0.05). This indicates that transcranial ultrasound thrombolysis combined with rosuvastatin treatment can improve patients' neurological function to a greater extent and enhance treatment efficacy.
(II) Comparison of blood lipid levels before and after treatment in the two groups
Before treatment, there was no statistically significant difference in blood lipid levels between the two groups (P>0.05). After treatment, the observation group had TG levels of (0.64±0.10) mmol/L, TC levels of (2.82±0.32) mmol/L, and LDL-C levels of (1.34±0.24) mmol/L, all of which were lower than those in the control group, with TG levels of (1.02±0.11) mmol/L, TC levels of (3.59±0.41) mmol/L, and LDL-C levels of (1.93±0.26) mmol/L. However, the HDL-C level in the observation group was (2.14±0.22) mmol/L, which was higher than that in the control group (1.97±0.20) mmol/L. The differences were statistically significant (P<0.05). This indicates that the combined treatment regimen can more effectively regulate patients' blood lipid levels and reduce the risks associated with dyslipidemia.
research discussion
(I) Pathogenesis and treatment key
As people age, lipid substances tend to deposit in the carotid arteries, leading to reduced elasticity and narrowed vascular lumens. This, in turn, can cause unstable blood supply to brain tissues, resulting in lesions and necrosis of some tissues due to ischemia and hypoxia. Currently, the key to clinical treatment of cerebral infarction lies in regulating blood lipids and dissolving thrombi to ensure blood perfusion to brain tissues.
(II) Mechanism of action of rosuvastatin
Rosuvastatin, as a statin drug, has the following main mechanisms of action:
1. Inhibiting 3-hydroxy-3-methylglutaryl-CoA (HMG-CoA) reductase, enhancing the uptake and catabolism of LDL-C, and inhibiting its synthesis in the liver, thereby reducing the concentration of cholesterol in plasma.
2. Reduce the cholesterol content on the platelet membrane and inhibit platelet aggregation.
3. Enhance the activity of superoxide dismutase, eliminate a large number of free radicals in the body, reduce oxidative stress response, and exert anti-inflammatory effects.
(III) Mechanism of action of transcranial ultrasound-induced thrombolysis
Transcranial ultrasound thrombolysis utilizes the high-frequency oscillatory effect and cavitation of ultrasound to break down thrombi within the vascular lumen through vibration, activate endogenous fibrinolytic activity, lyse fibrin, and subsequently reduce TG, TC, and LDL-C levels, transforming soft plaques into hard plaques to prevent plaque shedding. Additionally, ultrasound oscillation can heat blood, dilate blood vessels, promote blood circulation, and increase blood supply to brain tissue. The physicochemical effects of ultrasound can also enhance biological enzyme activity, promote aerobic oxidation of brain cells, activate neuronal cells, replace damaged neurons, and improve patients' neurological function.
(IV) Advantages of combination therapy
The results of this study indicate that the observation group exhibited a higher overall treatment efficacy compared to the control group. Specifically, the levels of TG, TC, and LDL-C were lower, while the level of HDL-C was higher in the observation group compared to the control group. This suggests that the combination of transcranial ultrasound thrombolysis and rosuvastatin treatment for ASCI is effective, contributing to the reduction of carotid plaque and lowering of blood lipid levels. The synergistic effect of these two treatment modalities further enhances the therapeutic outcome, bringing new hope to ASCI patients.
Source of this article:
Song Yuanyuan. Observation on the efficacy of transcranial ultrasound thrombolysis combined with rosuvastatin in the treatment of atherosclerotic cerebral infarction [J]. Journal of Practical Integrated Traditional Chinese and Western Medicine Clinical Practice, August 2021, Volume 21, Issue 16
Disclaimer: The content of this article is for reference only. For specific treatment plans, please follow the advice of a professional doctor.
Copyright Notice: The copyright of the article belongs to the original author. Reproduction without permission is prohibited.


